If you're looking for information about FTM top surgery, you probably already know what it is. What you may not easily find is what happens before, during and after surgery in practical terms: what questions to ask your surgeon, how to prepare your home for the post-operative period, when you can return to work or the gym, and what feelings are normal during recovery. This article is designed for exactly that point in the process: when you've already made your decision or are very close to making it, and what you need is straightforward, honest, straightforward information.
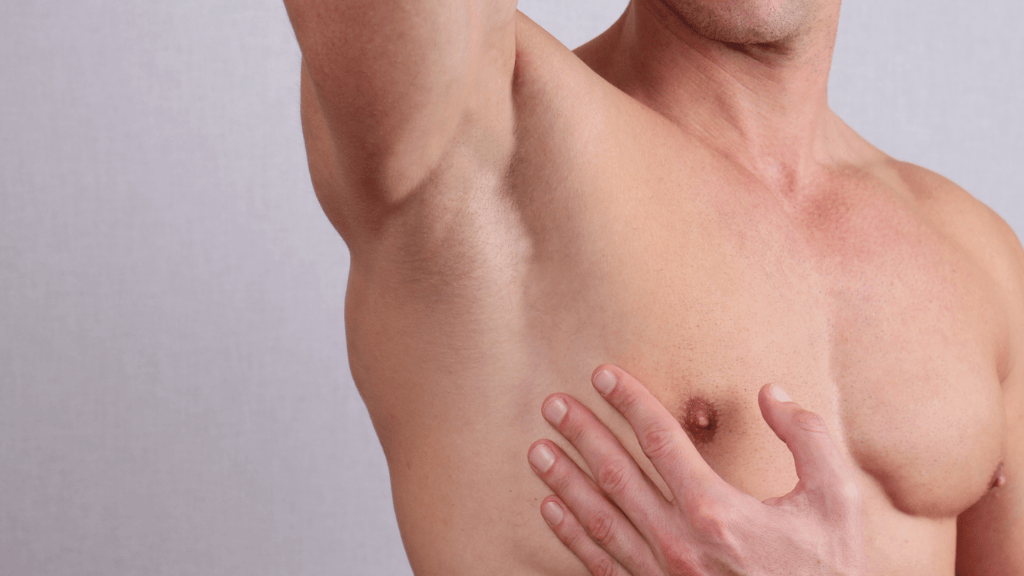
Mastectomy for trans men, known internationally as FTM (Female-to-Male) top surgery, is now a well-established procedure in gender-affirming plastic surgery. The results have improved enormously in recent years thanks to the evolution of techniques and greater specialisation of surgical teams. But like all surgery, the result does not depend solely on the surgical act: the preparation and aftercare are as important as the intervention itself.
Why pre-operative preparation makes a difference
One of the most common mistakes is to focus so much on finding the right surgeon and the date of the operation that the pre-operative phase is completely neglected. The preparation before the FTM top surgery directly influences three things: the safety during surgery, the speed of recovery and the final quality of the result.
These are the areas to pay attention to in the weeks leading up to the intervention:
Smoking cessation
Smoking is one of the most important factors compromising healing after any surgery. Nicotine reduces blood flow to the tissues, which slows cell regeneration and increases the risk of complications such as tissue necrosis or poor healing. The general recommendation is to stop smoking at least four weeks before surgery, although the longer you stay smoke-free before surgery, the better the outcome. This includes vaping and any other nicotine-containing products.
Review regular medication
Some medications and supplements can increase the risk of bleeding during surgery. Anti-inflammatory drugs such as ibuprofen or acetylsalicylic acid, certain blood thinners, high-dose vitamin E, and some natural supplements such as omega-3 or garlic capsules are usually stopped several days before surgery. It is essential to inform the surgeon and anaesthesiologist of everything you are taking, including supplements or herbal products, so that they can tell you exactly what you should stop taking and when.
Testosterone and surgery
If you are on testosterone, it is important to discuss with your endocrinologist and surgeon whether you should make any adjustments to your pre- and post-operative regimen. Testosterone is not a requirement for top surgery in Spain, but if you are already receiving it, some medical teams recommend adjusting the dose or timing of administration close to the date of surgery. Each case is different, so this decision should be made on a case-by-case basis with your medical team.
Preparing the body: nutrition and hydration
Arriving at surgery in good general condition speeds up recovery. Maintaining a balanced diet, rich in protein and vitamins in the weeks leading up to surgery helps the body to have the resources it needs to regenerate. Adequate hydration also plays an important role. Avoiding alcohol at least two weeks before surgery is another common recommendation, as it can interfere with anaesthesia and post-operative medications.
What to bring on the day of surgery: practical checklist
It may seem like a minor detail, but arriving well prepared on the day of surgery reduces stress and makes the early post-operative hours easier. Here are the things you should have ready:
- Comfortable, loose-fitting clothes with an open front: a zip or buttons at the front are a must, because raising your arms to put on a classic T-shirt will not be possible during the first few days.
- Comfortable underwear and socks: nothing tight and nothing that requires effort to put on.
- Medical documentation: the pre-operative report, the signed consent form and any other documents that the clinic team has given you.
- A trusted companion: you will not be able to drive or go home alone. This person should stay with you for at least the first 24-48 hours.
- Charged phone and charger: you will have plenty of time in the immediate postoperative period.
- No food or drink for the hours before the anaesthesiologist's instructions.
Recovery at home: how to organise yourself for the first few days
Discharge from the clinic usually takes place on the same day of surgery or the following morning, depending on the evolution of each patient. Arriving home with everything organised beforehand makes a real difference to how you experience those first few days.
Prepare your space before surgery
Expect that for the first three or four days you will have very limited mobility in your arms and upper trunk. This means that you will not be able to open jars, lift objects off the floor, reach high shelves or drive. Here are some practical things you can do before surgery:
- Place everything you need (medication, food, clothes, remote control, chargers) at an accessible height without having to stretch.
- Prepare light, easy-to-heat meals. Appetite may be reduced and mobility is limited for the first few days.
- Be prepared where you sleep: a slightly reclined position, with pillows to help keep your torso elevated, can reduce swelling and make the first few nights more bearable.
- If you have pets that jump or are very active, arrange for someone to help you look after them for the first few days.
Drains: what they are and how to manage them
At the end of the surgery, the surgeon places drains in the operated area to prevent the accumulation of fluid under the skin. These are small tubes connected to reservoirs that collect the fluid. They may be uncomfortable at first, but their function is important for the skin to adapt well to the new contour.
They are usually removed in the first 24 to 48 hours, at the post-operative check-up. The medical team will tell you how to care for them in that time: how to empty the reservoir, what colour and amount of fluid is normal, and when to contact them if something doesn't seem right.
Compression garments: why they are so important
After surgery you will need to wear a compression waistcoat or garment for several weeks, even to sleep in the early stages. This is not optional: compression helps the skin to retract and adapt to the new chest contours, reduces swelling and promotes more even healing. It is normal for it to be uncomfortable, especially in the first few days. But following this instruction to the letter is one of the things that most influences the final result.
One of the aspects that generates most doubts before surgery is what the scars will look like after the mastectomy and how they will evolve over time. Dr. Richard Fakin explains it clearly in the following video:
Week by week: what to expect during top surgery recovery
One of the most frequently asked questions before top surgery is: how long does it take to see the result? The honest answer is that the process is progressive and each week brings different changes. This is an indicative outline of how the recovery usually evolves:
Days 1 to 5: the most intense phase
The first few days are the most physically demanding. It is normal to feel discomfort, tightness in the chest area, some swelling and bruising. The painkillers prescribed by the surgeon help to manage the pain, which in most cases is more tolerable than anticipated. The most important thing at this stage is rest: sleep on your back, avoid any sudden arm movements and don't try to do more than your body will allow.
The breast will appear bandaged and covered with the compressive garment. It is possible that when you see the result for the first time, with swelling and inflammation, the image is not exactly what you expected. This is completely normal: the swelling distorts the contour a lot in these first days and does not represent the definitive result at all.
Week 1 and 2: regaining autonomy
From the seventh or tenth day, most patients begin to resume sedentary activities: working from home, walking short distances, cooking simple things. Post-operative check-ups during this period are important to assess how the scars are evolving and to remove stitches if there are any. The swelling is visibly decreasing, although it is still important to wear the compression garment.
Weeks 3 to 6: the big change
This is the phase when most patients start to see and feel the real result. Residual swelling continues to go down, the torso gains definition and the skin begins to adapt to the new contour. Around the second or third week, the medical team may recommend starting gentle mobility exercises with a physiotherapist to restore range of motion in the shoulder without compromising healing.
Intense physical activities, sports and weight lifting should wait until your surgeon gives you the go-ahead, which is usually between the fourth and sixth week. Returning earlier can compromise healing and the result.
From the third month onwards: the definitive result
The scars continue to evolve for months. They change from the initial red to duller tones and gradually flatten out. The definitive result of the surgery is assessed after three to six months, when all the inflammation has disappeared and the skin has finished adapting. The use of silicone creams or patches, applied according to medical indications, can significantly improve the appearance of the scars during this process.
In this video, Dr. Richard Fakin explains in a practical way what the postoperative period for top surgery is like and what to expect during the first few weeks:
The emotional impact of top surgery: what no one tells you
Most articles on FTM top surgery focus on the physical and technical aspects. But there is an emotional dimension that is equally important and should be understood before undergoing surgery.
For many trans men, the result of surgery brings a profound sense of relief, coherence and well-being that goes far beyond aesthetics. Activities that previously generated anxiety or discomfort, such as going to the swimming pool, playing sports without braces or simply looking in the mirror, are completely transformed. Many patients describe the first days after surgery as one of the most significant moments in their transition process.
At the same time, it is important to know that unexpected emotions can also appear: some sadness, a feeling of unreality or moments of insecurity, especially in the first days when the body is still swollen and the result is not visible. These reactions are normal. The healing process is slow, and the mind sometimes needs time to integrate such an important change. Having support from people you trust, from the trans community or from a mental health professional who understands the process can be a great help during this period.
How to choose the right surgeon for FTM top surgery
The choice of surgeon is probably the most important decision of the whole process. Not all plastic surgeons have specific expertise in FTM thoracic masculinisation. The difference between a natural and an unnatural result lies largely in the experience and aesthetic sensitivity of the surgeon performing the procedure.
Some criteria that should guide this choice:
- Demonstrable and specific experience in gender affirming surgery, not just oncological mastectomy or general breast reduction.
- Possibility to see real before and after cases of patients with a similar anatomy to yours.
- Time spent in the pre-operative consultation: a good surgeon will not rush you, will study your anatomy in detail and will explain clearly which technique is best suited to your case and why.
- A medical and patient care team that is accessible throughout the entire process, not just during surgery.
- Transparency about risks, outcome limits and possible revisions.
He Dr. Richard Fakin is a Swiss-Italian plastic surgeon with practices in Madrid and Zurich and an established track record in gender-affirming procedures. His approach combines precision surgical techniques with individualised planning that takes into account each patient's anatomy, skin type, breast volume and expectations. As a boutique clinic, the team takes the time to dedicate to each case to ensure a result that is proportional, natural and consistent with each individual's identity.
If you want to know the experience of patients who have already undergone this surgery with Dr. Fakin, you can read their testimonials at this page. Seeing real cases, with real results, is one of the most useful ways to gauge what to expect.
Frequently asked questions that no one dares to ask (but everyone has)
Can I have surgery without starting testosterone?
How long do I have to take time off work?
Will I lose nipple sensitivity forever?
When can I start exercising again and in what order?
Is it normal that I don't like the result at first?
Taking the step with information and the right equipment
Top surgery FTM is a surgery with very good results when it is performed with experience, with individualised planning and when the patient arrives well prepared. Practical information, that which goes beyond what appears in any clinical record, is what makes the difference between living the process with anxiety or with confidence.
If you are at that point where your decision is clear but you still have specific doubts about your case, the preoperative consultation with a specialist is the next logical step. Not to commit to anything, but to have someone in front of you who can study your anatomy, answer your real questions and help you understand what options you have and which ones suit you best.
Dr. Richard Fakin's team, with offices in Madrid and Zurich, treats this type of surgery with a personalised, technical and human approach. The first consultation is the best place to start.